Breast Reconstruction
Consultations offered at our seven convenient locations in Manhattan New York City, Princeton New Jersey, Scarsdale, Woodbury Long Island, Southampton, Smithtown and Boca Raton, Florida

Breast reconstruction is a surgical procedure to recreate one or both of a patient’s breasts using implants after a mastectomy. If a woman has breast cancer, it is necessary to remove the cancerous tissue via mastectomy or lumpectomy. Surgical removal of one or both breasts to rid the body of cancerous growths, can be an emotionally devastating experience. While this treatment has helped millions of women overcome cancer, some mastectomy patients find that their drastically altered new figures are a constant and unwanted reminder of an incredibly taxing period of their lives.
Breast reconstruction surgery can help restore a woman’s breasts, as well as her confidence and self-esteem, after a mastectomy. Dr. Stephen T. Greenburg has helped women around the world achieve the breast silhouettes they desire. If you would like to learn more about breast reconstruction, you may schedule an appointment and consultation by filling out this contact form, or by calling your nearest location today.
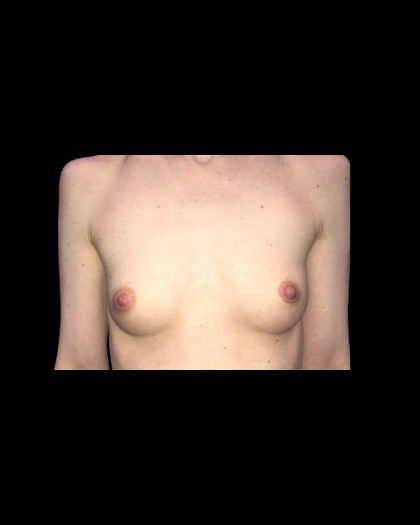
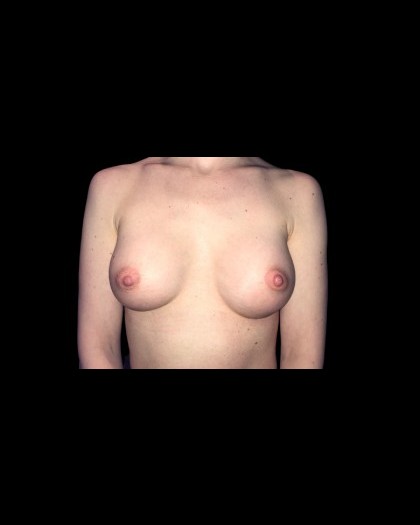
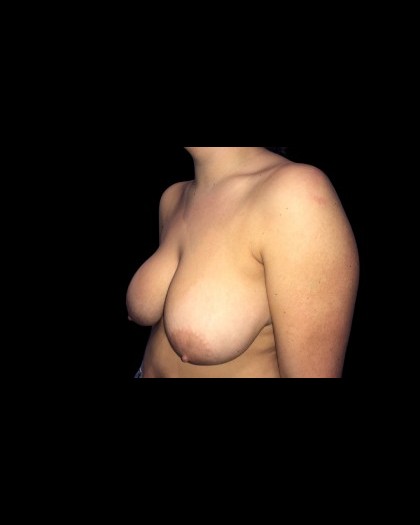
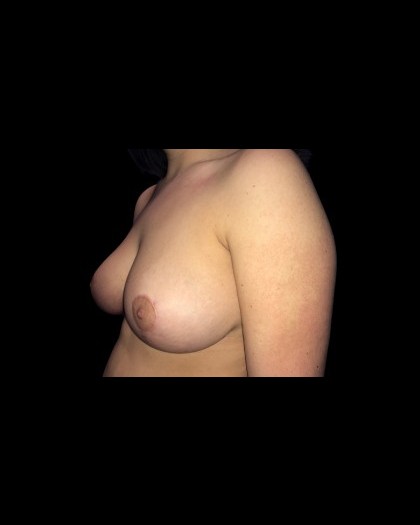
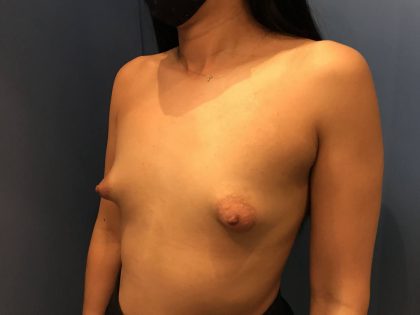
Before and After Photos
Contents
- 1 Before and After Photos
- 2 About Breast Reconstruction
- 3 Benefits of Breast Reconstruction
- 4 Tissue Expanders
- 5 Tissue Expander Procedure
- 6 Natural Breast Reconstruction Techniques
- 7 Autologous Breast Reconstruction
- 8 Breast Reconstruction Recovery
- 9 Post Procedure
- 10 Cost of Breast Reconstruction on Long Island
- 11 References
About Breast Reconstruction
After undergoing a mastectomy, patients often seek breast reconstruction surgery as an effective way to help restore the appearance of their breasts and renew their sense of femininity and beauty. Stephen T. Greenberg, M.D., F.A.C.S provides silicone breast implants at his practice for women seeking breast reconstruction with implants. Many women choose silicone implants because they provide the feel and appearance of natural breast tissue.
Breast augmentation and breast reconstruction are procedures that can have a profound effect on a woman’s figure, clothing options, and self-esteem. The kind of breast implant chosen for breast augmentation is central to the outcome, so it is very important to understand the unique attributes of silicone, saline, and the new gummy bear implants. To learn more about silicone implants and how they can help you achieve the breasts you desire, please contact our offices today.
Direct to Implant Procedure
Direct to implant breast reconstruction is one of the simplest and most effective techniques available for women after undergoing a mastectomy. This one-step solution places an implant in the treated area immediately after surgery with no need for a flap, graft or tissue expander. This allows patients to experience immediate recreation of the breast mound, and is often considered emotionally beneficial.
During the reconstruction procedure, the implant is placed on the chest wall behind the muscle, similar to the procedure used for breast augmentation. Patients have the choice of saline or silicone implants, as well as a variety of other choices, which can be discussed with their surgeon prior to surgery.
This procedure is performed immediately after the mastectomy, which reduces the operation costs and recovery times by combining the two surgeries into one. Direct to implant breast reconstruction is ideal for patients with good preservation of the breast skin after the mastectomy procedure that can support an implant. (1)
Benefits of Breast Reconstruction

Breast reconstruction surgery can effectively recreate the natural shape of the breasts, allowing women to restore confidence in their appearance. For patients who also want to achieve their former breast size and proportions, Dr. Greenberg can combine implant placement with reconstruction. Rebuilding the breasts with implants can:
- Improve the shape and size of the breasts
- Restore a patient’s natural curves
- Allow women to wear form-fitting clothes and bathing suits
- Provide symmetry to the breasts
- Restore the appearance of the nipple
For many women, their femininity and sexuality can be greatly affected by the removal of their breasts. Although their breasts will never be the same following a mastectomy or injury, reconstructive surgery with implants is an effective alternative to help women begin to feel whole again. During your private consultation, Dr. Greenberg will assess your breasts to determine the most appropriate approach to your breast reconstruction.
Tissue Expanders
After undergoing a mastectomy, many women do not have a sufficient amount of skin in the chest area to support an implant. In these cases, Dr. Greenberg can place a tissue expander to gradually stretch the skin and make room for an implant.
A tissue expander is a balloon-like device that is placed under the pectoral muscle. Following mastectomy, the doctor will inject a saline solution into the expander at regular intervals through a small valve located just below the surface of the patient’s skin. Once the tissue expander has sufficiently stretched the skin after about six to eight weeks, Dr. Greenberg will replace it with your breast implant.
Reconstructive surgery using a tissue expander and implant is often appealing because it requires less surgery than flap reconstruction. In general, patients undergoing reconstruction with implants can usually expect to reach full recovery after about six weeks.
Immediate Reconstruction
For some reconstruction patients, the use of a tissue expander is not necessary. If you have a sufficient amount of skin, we can perform immediate reconstruction and place an implant at the time of mastectomy, or at a later date.
Immediate breast reconstruction is more convenient than other reconstruction procedures since it does not require multiple surgeries. Whether you are considering breast reconstruction with implants during or after mastectomy surgery, you will want to ask your doctor whether the use of a tissue expander will be necessary. (2)
Tissue Expander Procedure
Breast reconstruction with tissue expanders is a multi-stage procedure that gradually expands the remaining natural breast tissue to create a pocket for the implant, eliminating the need for a flap or skin graft to cover the implant. During the first procedure, the tissue expander is placed on the chest wall and filled partially with saline. After an initial healing period, the expansion process begins by inserting more and more fluid into the device at regular intervals, often weekly.
For many patients, these appointments are coordinated with chemotherapy treatments, and take less than a minute to complete. The expanders each have a port in the front that can be easily accessed with a needle to inject the precise amount of fluid for each scheduled expansion. After expansion, patients may experience discomfort for up to 24 hours, which can be managed with Tylenol or other over-the-counter medications.
Once the expansion process is complete and a sufficient pocket has been created, the implant is placed during a second procedure. During this outpatient procedure, the tissue expander is removed and replaced with a breast implant. Patients can choose between several different implant types to pick the one that best fits their body and goals for surgery. This procedure takes about an hour to perform and usually takes place approximately a month after chemotherapy is completed.
The entire process usually takes four to six months to complete, after which patients can experience the benefits of reconstructed, natural-looking breasts with little to no reminders of cancer.
Natural Breast Reconstruction Techniques
With natural breast reconstruction, Dr. Greenberg will use skin, muscle, and fatty tissue from other areas of the body to reconstruct the breast. There are several different techniques available: (3)
- Transverse rectus abdominis myocutaneous (TRAM) flap – This technique involves an incision made across the lower belly from one hip to the other. Dr. Greenberg will loosen the skin, muscle, and fat in this area and move it into position to create the new breast. If the existing blood vessels are left attached to the tissue, it is known as a pedicle flap procedure. In some cases, patients are better suited to a free flap procedure where the tissue is removed from the existing blood supply and reattached to vessels behind the breastbone.
- Latissimus dorsi flap – During this technique, Dr. Greenberg will use tissue from the upper back, on the side of the breast that was removed. This tissue will be moved into place on your chest and used to create the new breast with the existing blood supply still attached.
- Deep inferior epigastric artery perforator (DIEP) flap – This technique is similar to a TRAM flap procedure, except the muscle tissue from your abdominal area is preserved. The DIEP flap surgery is one of the most frequently performed breast reconstruction surgeries
- Gluteal flap – The gluteal flap technique uses skin, muscle, and fatty tissue that is taken from the buttocks to reconstruct the breast. The tissue will be reattached to the blood supply under your arm or behind the breastbone.
- Transverse upper gracilis (TUG) flap – This technique is similar to a gluteal flap, except the skin, fat, and muscle is taken from one of your thighs. The tissue will be moved to your chest to create the new breast and reattached to the existing blood supply.
Autologous Breast Reconstruction

After tissue expanders, skin and/or muscle flaps are the next most common form of reconstruction. This natural breast reconstruction method takes skin and muscles, usually from the abdomen (DIEP or TRAM) or back (Latissimus), to recreate a breast. A DIEP flap is a complex procedure that utilizes microsurgery to take abdominal tissue with its blood vessels and transplant it onto the chest wall. In this new location, the blood vessels are reconnected under a microscope to blood vessels in the chest. The skin flap can then be fashioned into the shape of a breast.
During the transverse rectus abdominis myocutaneous (TRAM) flap reconstructive procedure, an incision will be made in the abdomen to lift layers of skin, fat, muscle and blood vessels. These tissues may then be cut from the body and reattached in the chest (a “Free TRAM”), as performed for the DIEP flap, or a tunnel is created under the skin to relocate the tissue to the breast area (“Pedicled TRAM”). The breast mound is then carefully reshaped with these tissues.
The DIEP and TRAM flap breast reconstructions are able to produce a breast that looks and feels natural, and provides the added benefit of a flatter abdomen from the tummy tuck procedure.
The latissimus dorsi (LD) flap is composed of soft tissue. During an LD flap reconstruction, a muscle and skin flap is taken from the back and moved through a tunnel to the front of the chest. The LD flap receives its blood supply from the thoracodorsal artery, which remains attached after surgery to ensure proper blood flow. This procedure most often requires a tissue expander. (3)
Oncoplastic Lumpectomy
If a patient requires a large lumpectomy that will significantly alter the shape of the breast, an Oncoplastic Lumpectomy Reconstruction procedure will be recommended. Dr. Greenberg will treat the procedure somewhat like a breast reduction or breast lift, in that he will be removing tissue and maintaining proportion in both breasts.
Once the malignancy has been removed, the breast is reshaped and the nipple aligned, Dr. Greenberg will move on to the other breast to remove a similar quantity of tissue and shape it symmetrically. Lumpectomy reconstruction allows a patient to obtain all necessary breast work in one procedure.
Breast Reconstruction Recovery

One of the most important aspects of undergoing breast reconstruction surgery is being both mentally and physically prepared for your recovery. Treatment planning can be an emotional and potentially stressful time for patients, as well as the post-operative phase.
To help make the process of breast reconstruction recovery as easy and comfortable as possible, Long Island, New York, surgeon Dr. Greenberg will guide each patient through what to expect, offering recommendations and tips. He will also conduct a series of follow-up appointments to check on your progress and address any concerns that arise.
Although the recovery period after breast reconstruction requires patience, some discomfort, and multiple weeks of downtime, patients can remain focused on healing by envisioning their final outcome.
Planning for Recovery
Depending on the type of reconstruction we recommend, using either implants or your own tissue, complete recovery can take up to two months. Prior to undergoing surgery, patients should be well prepared both mentally and by making accommodations at home. For example, you should plan on stocking your fridge with nutritious foods. You should also reach out to family, friends, and caregivers since a good support system can help make the downtime and recovery less stressful and ensure your comfort.
Post Procedure
Immediately following the reconstructive procedure, patients will experience muscle soreness, swelling, bruising, and some level of discomfort. Drains may be inserted beneath the skin to facilitate healing, and Dr. Greenberg will provide instructions on how to keep the area clean. To further promote the healing process, we may recommend:
- Minor Activity: Proper rest is important during your recovery, but every two to three hours you should walk for a few minutes to encourage circulation
- Elevating Your Head and Chest: Using pillow to prop yourself up can minimize swelling, as can elevating your knees if you have undergone a TRAM (transverse rectus abdominis myocutaneous) or DIEP (deep inferior epigastric artery perforator) flap procedure.
- Medication: To minimize pain and discomfort, Dr. Greenberg will prescribe medication and explain instructions to their use prior to your procedure.
- Expanding Your Lungs: To prevent fluid from accumulating in your lungs, which can lead to pneumonia, it is important to take a series of deep breaths every hour. Patients should also try to cough a few times per hour, placing a pillow over their stomach to reduce discomfort.
- Light Eating: Patients should eat light foods such as jello, soup, and crackers for the first few days or until they can build up to more substantial and solid meals.
When You Should Contact Your Doctor
It is important to contact Dr. Greenberg if you are experiencing any type of intense discomfort, a high fever, severe nausea, vomiting, excessive bleeding, or fluid seeping from incisions or drains. These symptoms can indicate infection or other complications. You should also alert us of any unexpected reactions to medications or side effects that were not discussed in your pre-operative visit.
Cost of Breast Reconstruction on Long Island
Breast reconstruction with implants is a highly personalized surgical procedure. The cost of the surgery will vary between patients based on a variety of factors. Our team will let you know what the expected price will be during your consultation.
Cancer survivors deserve to enjoy their lives to the absolute fullest. If you believe your enjoyment of life could be enhanced through breast reconstruction surgery, Dr. Greenberg can provide compassionate consultation and beautiful results. Contact us online or call to learn more about how we can assist you with this process.
References
- Rocco N, Rispoli C, Moja L, et al. Different types of implants for reconstructive breast surgery. The Cochrane Database of Systematic Reviews. 2016;2016(5). doi:https://doi.org/10.1002/14651858.CD010895.pub2
- Schmauss D, Machens HG, Harder Y. Breast Reconstruction after Mastectomy. Frontiers in Surgery. 2016;2(2). doi:https://doi.org/10.3389/fsurg.2015.00071
- Breast Reconstruction After Mastectomy. National Cancer Institute. Published February 24, 2017. Accessed October 19, 2023. https://www.cancer.gov/types/breast/reconstruction-fact-sheet